Quick Facts
We are pleased to introduce recipients of the CDAF-Relink grant. From health departments to non-profit organizations and healthcare institutions, our grantees reflect the spectrum of organizations working to reconnect individuals living with hepatitis B and C in the United States to care.
| Round | Amount Committed | Grantees | States |
|---|---|---|---|
| 1 | $1.6M | 13 | 11 |
| 2 | $1.7M | 11 | 10 |
| 3 | $782K | 6 | 6 |
| 4 | $2.4M | 14 | 10 |
Grantee Locations
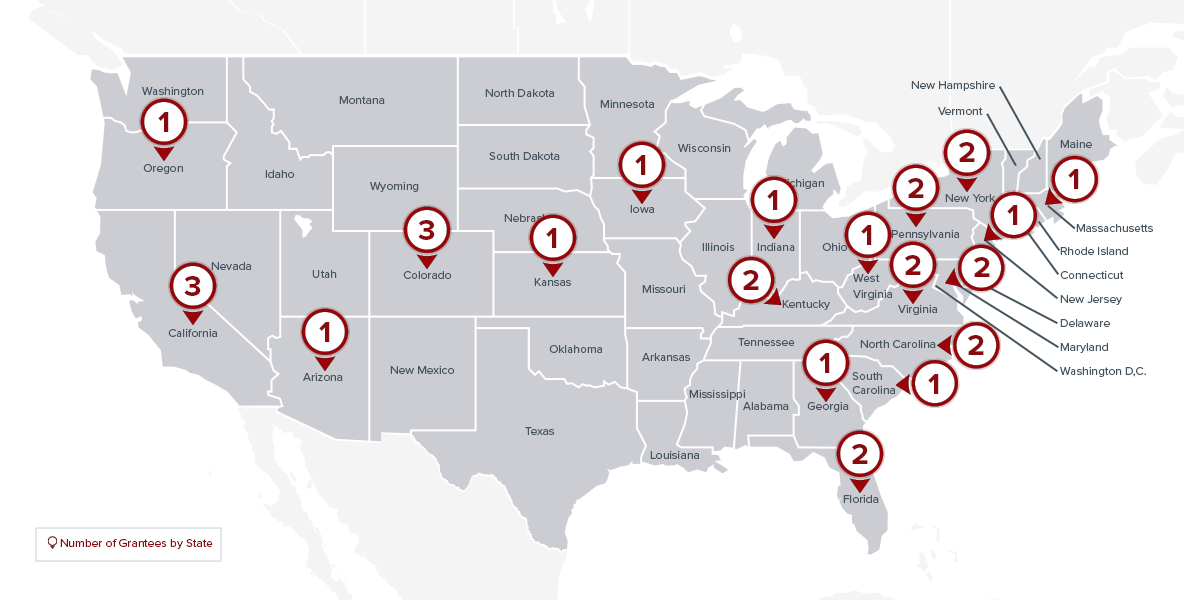
Grantees
The AIDS Leadership Foothills-area Alliance (ALFA) stands as one of the bulwarks against the devastating impact of the opioid addiction crisis in the Appalachian foothills area of North Carolina. The ALFA relink program focused on hepatitis C infected individuals experiencing housing insecurity or who have a history of injection drug use. Faced with challenges like distrust of medical providers, limited transportation access, lack of health insurance and itinerancy, the program investigated and established evidence-based protocols for reengaging and incentivizing people from these vulnerable populations who have fallen out of care.
The Arizona Department of Health Services relink program highlights the critical role departments of health can play in the effort toward viral hepatitis elimination in the United States. Grant funding will support workflows which leverage access to Arizona’s Health Information Exchange and other large databases to identify and reconnect diagnosed but untreated hepatitis C infected individuals from vulnerable populations like current or former injection drug users, as well as the general population. Their long reach is bolstered by the Hepatitis C RapidLink protocol which focuses on strengthening relationships between patient navigators, testing centers, and treatment clinics.
The Asian Health Services relink program focused on reconnecting immigrant patients living with hepatitis B or C to care and treatment. As an organization well embedded in the Asian American and immigrant community of Alameda County in the San Francisco Bay Area, their community health advocate model of care lived up to their mission to provide culturally and linguistically appropriate health care to their community.
West Virginia remains one of the states most affected by the opioid addiction crisis, with the accompanying epidemic of infectious diseases including hepatitis B and C. The Bluestone Health Association relink grant supports the organization’s work on the frontlines. The program concentrates on rural, low income, formerly justice-involved and homeless populations, as well as individuals recovering from substance abuse. This ensures the most vulnerable get the most support.
Individuals experiencing housing insecurity and who are infected with hepatitis B or C face unique challenges. Equipped with over a decade of experience, the award-winning Boston Health Care for the Homeless Program Hepatitis C initiative leverages their network of shelter-based clinics and street outreach services to re-engage still vulnerable individuals in their service area. The relink grant will broaden their reach, supporting data driven workflows and boosting community outreach efforts.
The Carillion Clinic relink program targets individuals diagnosed with hepatitis C but who have been lost to follow up from various settings across the Carillion Health System. As one of the largest healthcare providers in Southwest Virginia, their scope is both rural and urban, ensuring broad coverage for a region still grappling high hepatitis C infection rates linked to the opioid crisis. The grant will enable them to expand existing services by refining the accuracy of their hepatitis C patient registry, improving workflows, and incorporating peer-supported community outreach into their model.
Central City Concern is a Federally Qualified Health Center operating out of multiple locations across the Portland metro region in Oregon. The Hepatitis C Elimination Program specializes in screening for and treatment of hepatitis C. The interdisciplinary team collaboratively works to serve people who are below the federal poverty level, experience houselessness or who are in recovery. The team conducts outreach, has established partnerships with Opioid Treatment Programs and other social service organizations, as well as manages two clinic sites. Grant funding will help expand service provision to temporary housing while in treatment, and accommodate additional support for patients to feel empowered to cure their hepatitis C.
The Colorado Department of Public Health and Environment’s relink program uses access to statewide hepatitis C RNA data to identify and re-engage individuals who previously had a positive RNA result but no subsequent negative result on record. To strengthen engagement, dedicated case ascertainment specialists conduct outreach and connect individuals to hepatitis C treatment visits, transportation assistance, and targeted incentives. The program also benefits from partnerships with the Department of Corrections and a broad network of low‑barrier providers, which together help embed re‑engagement activities into the state’s existing public health infrastructure.
The Community HealthNet relink program targets populations disproportionately affected by hepatitis C in Northwest Indiana. The program adds to their decades of experience investigating and managing suspected and potential cases of hepatitis C. Grant funding will support the hiring of specialist team members to further relinkage efforts, as well as the development of more streamlined data management processes.
The relink program of the Florham Park Multispecialty-Center for Asian Health at the Cooperman Barnabas Medical Center identifies patients with untreated hepatitis B or C within the RWJBarnabas Health System, with a focus on patients positively diagnosed during pregnancy. Historically, this latter group has shown vulnerability to linkage failure in the post-partum period. The program’s partnership with local health departments and other community health organizations ensures a comprehensive and sustainable model of care for the perinatal and general population.
Based in the Denver metro area, Denver Health Medical Center serves as the hub of a network of neighborhood based Federally Qualified Health Centers which cater to vulnerable populations including people living with substance use disorders. Grant funding will supplement efforts within this multi-faceted network to relink individuals with untreated hepatitis B and C from primary care, specialty clinics and the Outpatient Behavioral Health Services unit. In the philosophy of “meeting patients where they are,” their program’s approach combines enhanced navigation support, face-to-face interactions, and e-consults with low-barrier to care options.
Family Health Centers of San Diego is a Federally Qualified Health Center with almost a decade of experience providing hepatitis B and C care coordination in San Diego County. Their relink program aims to deepen their impact by improving patient registries, relinkage workflows, and better targeting comprehensive care. Their proximity to the US-Mexico border and wide network of fixed site clinics and mobile units ensures comprehensive coverage for populations most affected by hepatitis B and C.
First Choice Primary Care was established by a group of community volunteers. The organization maintains a policy of providing primary care to anyone, regardless of their ability to pay. Grant funding will support the creation of an official registry of individuals infected with hepatitis B or C and the implementation of a patient navigation service to facilitate relinkage to care. With six clinical sites which service large swathes of rural Georgia, their efforts will meet the needs of this easily overlooked population.
The Health Betterment Initiative (HBI), formerly the Hepatitis B Initiative of Washington DC, is one of the DMV region’s most committed providers of hepatitis B and C case management, with a focus on immigrant and other vulnerable populations. Their relink program enhances this effort, combining a collaborative, compassionate approach with linguistic and cultural sensitivity to help patients overcome healthcare barriers. Additionally, the program offers Hepatitis Delta education to raise awareness among individuals living with hepatitis B, highlighting HBI’s steadfast dedication to supporting their community.
The Iowa Department of Health and Human Services relink program offers further evidence for the centrality of health departments in the effort towards hepatitis C elimination in the United States. Grant funding has enabled the existing Prevention Navigation Team to widen their scope by utilizing state health records to identify and contact untreated hepatitis C infected individuals. This involved onboarding a Re-engagement Specialist and developing a Re-engagement Program Manual which will assist other jurisdictions in replicating the developed protocols. The program’s successes have already contributed to the program recommending a permanent position to continue important reengagement work at a broader level.
The Kansas Department of Health and Environment relink program expands their existing Viral Hepatitis Linkage to Care (VHLTC) program. VHLTC collaborates with the Infectious Disease Epidemiology and Response (IDER) Section, targeting newly diagnosed individuals and reengaging previously diagnosed but untreated individuals. Navigators perform initial follow-up and provide patient education, navigation, and referrals. However, their activity was limited to individuals aged forty-five and under. Grant funding will expand their scope to cover the total population of diagnosed but untreated hepatitis C infected individuals.
The University of Southern California’s Hepatitis B relink program builds on the work of the HBV BRIDGES program, a public health partnership with Los Angeles County aimed at improving linkage to care for adults with chronic hepatitis B. Using a countywide laboratory‑based registry, the program identifies diagnosed but untreated individuals and conducts multilingual phone outreach to assess awareness, provide education, and encourage reengagement in care. Grant funding will expand a successful pilot that demonstrated strong feasibility and benefits from established infrastructure, multilingual volunteer capacity, and ongoing data support.
Kingman Regional Medical Center’s rural hepatitis C program serves the Mohave County community through navigator‑led outreach paired with a pharmacist‑driven treatment model. Building on the Disease Management Clinic’s 82.3% confirmed cure rate from 2020–2024, the program leverages cross‑department data integration, financial support, and collaborative practice agreements to reduce barriers to care. Program results will help strengthen the case for specialty pharmacy designation to enable on‑site dispensing and support expanded partnership with the County’s Mobile Health Unit to reach patients in remote areas.
The Los Angeles County Department of Public Health Relink Program uses a countywide database and information from housing programs to identify and locate individuals living with hepatitis B and C who are lost to follow-up. This approach relies on stable housing, trusted relationships, and coordinated public health infrastructure to overcome longstanding barriers to care. Grant funding will support the hiring of a dedicated medical caseworker and the development of streamlined care coordination processes.
The Montefiore Medical Center Hepatitis C Treatment Network has combined partnerships with the New York City health department and organizations collaborating with communities heavily affected by viral hepatitis in the Bronx, New York since 2016. Grant funding will augment an existing approach that integrates best practice alerts, reflex testing, point-of-care testing in high-vulnerability settings, outreach, and navigation support. Funding will also support agency partnerships to strengthen linkage to and engagement in care for the hardest-to-reach populations living with viral hepatitis. Specific innovations from the relink program involve further information technology, data science, and health systems integration.
LEAP, the Liver Education and Action Program of Mount Sinai’s Institute of Liver Medicine is a pioneer in efforts to relink diagnosed but untreated individuals with chronic hepatitis B and C in the United States. Their approach combines sophisticated case-finding algorithms, intensive chart reviews, collaboration with emergency department teams and primary care providers, and empathetic patient outreach informed by motivational interviewing techniques to encourage appointment adherence. Their reach spans the Mount Sinai Health System in the greater New York City metropolitan area. This gives them access to multiple vulnerable populations including immigrant populations, as well as the general population.
The Nevada Department of Human Services’ ReLink program partners with health centers across the state to connect individuals with untreated hepatitis C to comprehensive, patient‑centered care. Many of the individuals with untreated hepatitis C are those who are unstably housed, incarcerated, uninsured, or who use injection drugs. The program’s dedicated patient navigator will conduct direct outreach, warm handoffs to clinical teams, and tailored referrals. Nevada will explore the feasibility of sustaining the re‑engagement efforts, through insights from the program to guide the development of a statewide online referral portal for follow‑up and referral based on laboratory results.
The New York City Health Department’s relink program uses a surveillance‑driven, iterative data‑to‑care model to re‑engage individuals living with hepatitis B and C who have fallen out of care. The program prioritizes a wide range of vulnerable populations, including individuals with HIV coinfections, recurrent HCV infection, recent testing at substance‑use treatment facilities, pediatric and adolescent patients, people of childbearing age, and those who are justice‑involved. Grant funding will support two additional linkage specialists, expanding the program’s capacity for multimodal outreach, intensive care coordination, and warm handoffs to community providers.
North East Medical Services (NEMS) is a federally qualified health center in the San Francisco Bay Area that serves a large non-U.S.-born Asian population at increased risk for hepatitis B infection. NEMS’ ReLink patient re engagement program focuses on individuals living with chronic hepatitis B who are diagnosed but untreated, missing a baseline fibrosis assessment, indicated for hepatitis B treatment, or lost to follow up. Through culturally-tailored education and focused interventions, NEMS aims to improve hepatitis B care management in the primary care setting.
The Northern Kentucky Independent District Health Department (NKY Health) relink program operates across community, clinic, and mobile settings to identify and re‑engage individuals living with hepatitis C who are lost to follow‑up. The program’s approach combines phone, mail, and text outreach with same-day GeneXpert RNA testing and a dedicated linkage team to immediately reconnect diagnosed‑but‑untreated individuals to care. Modeled on NKY Health’s successful Ryan White HIV linkage system, grant funding will support the program’s expansion to provide comprehensive case management for re-engaged participants.
The Norton Healthcare relink program sought to determine optimal relinkage pathways for individuals from vulnerable populations who are diagnosed but untreated for hepatitis B or C. Their three-pronged approach compared an emergency department-based alert system for untreated individuals to rigorous chart reviews coupled with telephone outreach by patient navigators and community-based nurse navigation paired with direct referrals and telehealth options. Findings supported the validity of community-based navigation and direct referrals.
The relink grant enables Philadelphia FIGHT’s Education, Outreach and Navigation Services (EONS) to re-engage the almost 1500 diagnosed but untreated Hepatitis B and C infected individuals in their system. In collaboration with local health departments, their program pioneered intensive investigations to ascertain the status of affected individuals. The relink program’s successes are now established as the “Call 2 Care” initiative applicable to all FIGHT patients regardless of illness type, who have not been seen in 18 months or more.
The Prisma Health relink program further elaborates on the efforts of the Prisma Health Addiction Medicine Center’s highly experienced substance uses disorder case management program. Their approach adapts an assertive community engagement model developed for peer-based substance use disorders interventions to hepatitis C relinkage efforts targeting the general population as well as vulnerable populations. Grant funding supports the implementation of efficient and cost-effective strategies and the establishment of best practices.
The Sentara Martha Jefferson Medical and Surgical Associates Virginia Hepatitis C Education and Patient Connection (HEPC) relink program operates within the broader framework of ongoing state-wide initiatives to improve access to high-quality hepatitis C care. The team draws on eight years of experience in outreach and hepatitis C care coordination among formerly incarcerated individuals, those with current or past substance use, and other heavily impacted populations. The current program focuses on the general population within the Sentara Health System, using the convenience of treatment via telehealth and an innovative hepatitis C referral network for those preferring to receive care in a clinic setting.
The Virginia HEPC and Roanoke City & Alleghany Health District (RCAHD) relink program builds on earlier Virginia HEPC efforts using a coordinated hub‑and‑spoke model led by RCAHD. The program re‑engages individuals living with hepatitis C in southwest Virginia, focusing on high‑burden and underserved groups such as people who use drugs, rural communities, and justice‑involved individuals. It uses proven approaches — including stigma‑reducing peer outreach, streamlined referrals with telemedicine access, real‑time data‑to‑care tracking, and clinician training — to improve linkage to care and treatment.
The Health & Hospital Corporation of Marion County (dba Eskenazi Health) Relink program uses a Disease Intervention Specialists (DIS) driven linkage‑to‑care model to find and re‑engage individuals diagnosed but untreated for hepatitis B and C. Grant funding expands the ability of the DIS team to use a wide range of tools to locate patients, conduct targeted outreach, and connect them with appropriate services. This outreach is reinforced by active case management across the care cascade to support treatment completion and retention. Program results will advance efforts to secure long‑term DIS capacity dedicated to re‑engaging individuals with untreated hepatitis B and C.
The TruReach relink program focuses on reengaging vulnerable individuals living with hepatitis B or C in rural Pennsylvania. In the spirit of “meeting patients where they are”, their approach employs community mobile clinics, telemedicine, and in-person outreach to residential and outpatient substance use facilities. TruReach staff are skilled in connecting patients with available resources. This includes assistance with navigating the path to affordable treatment access, referrals to community-based organizations that addresses social determinants of health, and other support. Their program covers forty-three rural counties and thirteen urban counties across Pennsylvania, filling a gap created by the lack of capacity of local health departments.
UC San Diego Health’s Beyond Screening relink program is an emergency department–based initiative designed to identify and re‑engage individuals with hepatitis C from vulnerable populations, including people who are unhoused and people who inject drugs. Its placement in the emergency department enables immediate linkage to a multidisciplinary care team, facilitating rapid initiation of therapy, streamlined insurance processes, and coordinated navigation. The program also supports hard‑to‑reach patients by providing mobile phones to maintain contact and ensure consistent follow‑up.
The University of Chicago Medicine’s relink program uses a multipronged strategy to identify and re‑engage individuals living with Hepatitis C, drawing patients from the emergency department, inpatient units caring for medically complex individuals, and mobile outreach efforts serving people who use drugs and those experiencing homelessness. The program offers counseling, expedited therapy, and mobile services for laboratory testing and medication delivery. Supported by interdisciplinary coordination, strong collaboration with state public health partners, and a record of successful treatment, the program is positioned to lay the groundwork for post‑grant re‑engagement activities that advance innovative, community‑based care models addressing health disparities.
Inpatient settings remain a missed opportunity for re-engaging diagnosed but untreated hepatitis B and C patients to care. Accordingly, the relink program of University of Colorado – Denver’s Division of Hospital Medicine seeks, primarily, to connect with untreated hepatitis C infected individuals who previously experienced hospitalization for reasons unrelated to their infection. The program also expands ongoing efforts to connect with individuals diagnosed during acute care hospitalization but not linked to treatment at the time of discharge.
The CHIP Prevention Program relink initiative brings much needed hepatitis C case management to vulnerable populations like people who use injection drugs, unhoused or justice involved individuals, and baby boomers in Colorado’s southern and mostly rural counties. The program is supported by a partnership with the Colorado Department of Public Health and Environment. Grant funding is directed towards patient incentives, hepatitis C provider training, and capacity building to encourage confirmatory testing and linkage to treatment.
The relink program of the University of Florida College of Medicine, Jacksonville’s Hepatology Department focused on urban and socioeconomically disadvantaged individuals infected with hepatitis C. The program is the first of its kind for the department. Using an approach that combined chart reviews and outreach to both infected individuals and, when available, their primary care providers, the program sought to assess optimal pathways to relinkage. Outcomes revealed that the paucity of access to reliable communication technology, transportation, as well as poor education about the health implications of hepatitis C have a significant and detrimental impact on this population.
Having built one of the nation’s largest adult non-targeted Hepatitis C screening and linkage to care programs in 2018, the University of Kentucky Research Foundation team implemented CURES (Cascade Utilizing Routinized screening through treatment to Eliminate Syndemics), a novel, emergency department based, pharmacy-led intervention. The CURES model both radically reduced time from diagnosis to treatment by over 90% and increased treatment from 10% to 60% of eligible patients. The relink program expands the system’s reach to include and re-engage people from vulnerable populations and the general population who were diagnosed with hepatitis C before or outside the implementation of CURES.
The University of Maryland School of Medicine’s Institute of Human Virology’s relink program is situated in the institution’s community health outreach and engagement arm, the JACQUES Initiative. With over two decades of experience in successful, innovative HIV and hepatitis C case management, the JACQUES Initiative staff are well-positioned to re-engage hepatitis B and C infected individuals who have fallen out of care, especially those from structurally vulnerable populations. Their approach fuses retrospective chart reviews with telephone and other technology facilitated outreach, and referrals to clinical programs across not only Baltimore City but the state of Maryland. Grant funding also supports connections to public assistance and community resources.
The relink program of the University of Miami Division of Infectious Diseases focuses on untreated hepatitis B and C infected individuals diagnosed in outpatient, emergency department and inpatient settings across the University of Miami Health System. Their approach melds chart reviews with callbacks and intensive navigation tailored to varied patient cultural, behavioral and social backgrounds. Grant funding will enable a pivot toward more assertive re-engagement to care with emphasis on liver cancer prevention awareness. Program outcomes will also support attempts to formalize long-term, system-wide hepatitis B and C micro-elimination and hepatitis-related cancer prevention services.
The multi-disciplinary team at the University of North Carolina, Chapel Hill relink program focuses their efforts primarily on vulnerable population (substance abuse recovery, post-incarceration, immigrant) within their cohort of pregnant and postpartum individuals infected with hepatitis B or C. The team follows infants born to people living with either virus to ensure testing and, if necessary, referral to care, yielding insights into challenges faced by this sub-population. Further efforts are directed toward the general population of diagnosed but untreated individuals within the wider University of North Carolina Health System, encompassing fifteen hospitals across the state.
This relink program is a collaboration between the Los Angeles County Department of Public Health and the Klausner Research Group of the University of Southern California’s Department of Population and Public Health Sciences. It combines access to the Los Angeles countywide hepatitis C registry and patient navigation by trained case workers with linkage to treatment to local community-based providers. In addition to augmenting patient navigation efforts, grant funding enables the development of a case management toolkit with protocols and procedures for staff, training manuals, and a resource guide.
The West Virginia University and Community Care of West Virginia (CCWV) relink program expands efforts to identify and re‑engage individuals diagnosed with hepatitis C but untreated across CCWV’s primary care and addiction medicine settings. The program leverages EHR‑driven patient identification, structured outreach, coordinated care navigation, and telehealth‑based treatment access. Supported by statewide hepatitis initiatives, expanded treatment availability, multidisciplinary collaboration, and sustainable workflows, the program aims to strengthen long‑term linkage to care and improve population‑level health outcomes.